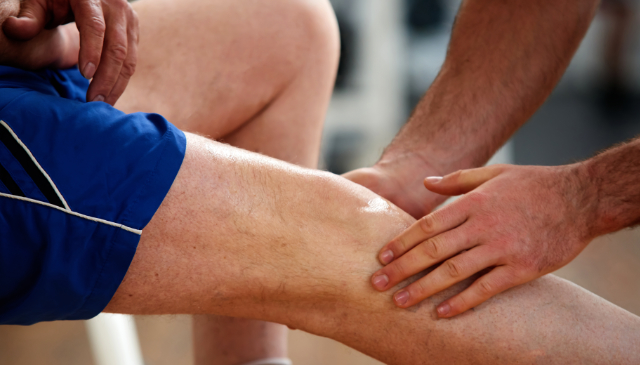
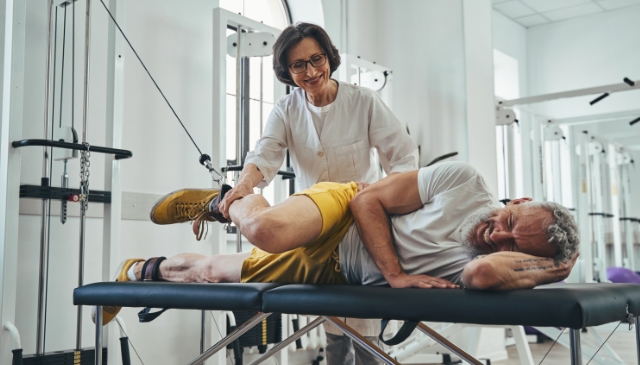
Are Deep Squats Really as Bad as We Think?
Ever heard the saying, âNever squat past your kneesâ? It's a common piece of advice, often given with the best intentions of protecting those precious joints. But what if we told you that going deeper in a squat might actually be beneficial for your knee health? For years, many believed that deep squats–where your thighs […]