Reclaiming Your Grip: The Power of Hands-On Therapy for Tennis Elbow
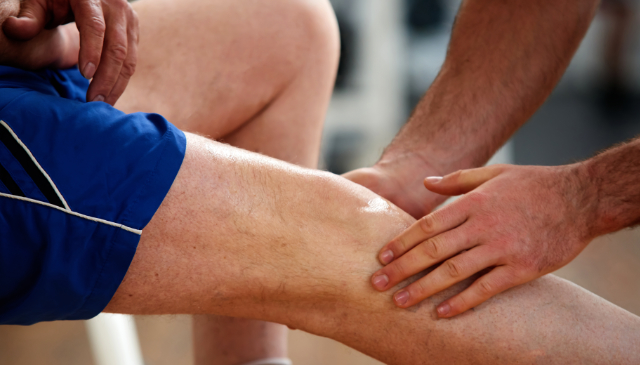
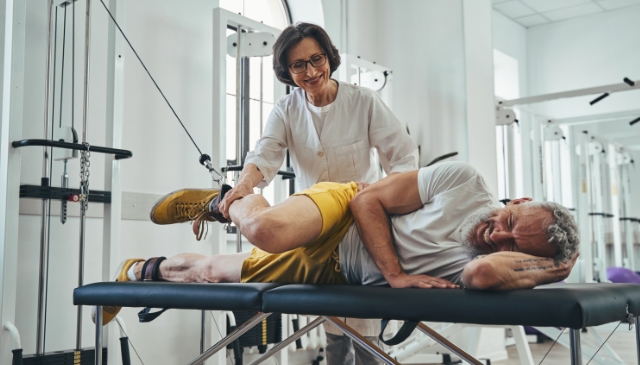
Ever tried to swing a racket or lift a coffee mug, only to feel a sharp twinge in your elbow that said, âNope, not todayâ? That sensation may be lateral epicondylitis–more commonly referred to as tennis elbow–announcing its presence like an uninvited guest. It's a pesky condition that doesn't just haunt tennis players, as anyone […]